
Periodontics
Periodontics deals with the treatment of, after caries, second most common disease of the mouth and teeth – periodontal disease, known in the people as periodontosis. This is a progressive disease, which overtakes the whole support of the tooth apparatus (gingiva, cementum, periodontium and bone). It begins with gingivitis – inflammation of the gums around the teeth (redness, swelling, bleeding) and later attacks and deeper tissues.
What is the cause of periodontitis?
It is thought that the main cause of periodontal disease is a dental plaque. It contains bacteria, which by their toxins damage the tooth-supporting apparatus. If plaque is not removed regularly, it is implanted in minerals from saliva, it becomes firm and calculus is formed. It’s a tough dental plaque, which further causes accumulation of plaque (due to uneven surfaces), and mechanically (pressing the gums) potentiates the ignition. Of course, many other factors support the development of this disease. Irregular tooth position, inadequate filling, dentures, and poor jaw relationship, also affect on the state of the support apparatus, so a complete repair of the mouth and teeth is necessary for the treatment of periodontitis.
Symptoms of periodontal disease
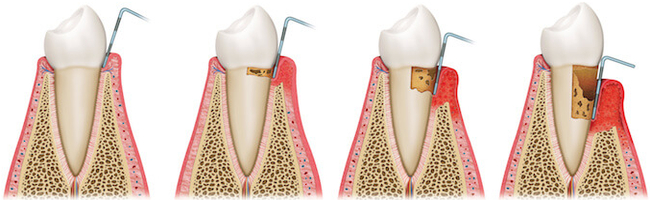 Parodontopathy begins almost imperceptibly. Patients often do not know that they have this illness until their dentist in control does not draw attention to the initial changes. One of the first symptoms that patients notice is bleeding when washing teeth or using a dental floss, but the sensitivity of the tooth to cold, pain when chewing, halitosis. In advanced stages, periodontal disease leads to significant withdrawal of the gums and bone loss. This results in the appearance of periodontal abscess (an infection that comes from deep periodontal pockets, unavailable for cleaning), loosening, pathologic tooth migration (tooth movement that manifests because of the appearance of the space between the teeth in places where previously did not exist) and loss of one, several or all teeth.
Parodontopathy begins almost imperceptibly. Patients often do not know that they have this illness until their dentist in control does not draw attention to the initial changes. One of the first symptoms that patients notice is bleeding when washing teeth or using a dental floss, but the sensitivity of the tooth to cold, pain when chewing, halitosis. In advanced stages, periodontal disease leads to significant withdrawal of the gums and bone loss. This results in the appearance of periodontal abscess (an infection that comes from deep periodontal pockets, unavailable for cleaning), loosening, pathologic tooth migration (tooth movement that manifests because of the appearance of the space between the teeth in places where previously did not exist) and loss of one, several or all teeth.
What is a periodontal pocket and how it occurs?
In patients with healthy gums, there is a small space between teeth and gums, called gingival sulcus and into which can be entered with a dental instrument (probe) to a depth no greater than 2-3 mm. When the inflammation of the gums occurs (gingivitis), this area is deepened due to the swollen gums and occurs the so-called gingival pocket. This expression should not be mixed with a periodontal pocket, which results from bone loss and by displacing the bottom of the space between the tooth and the gums to a lower level (closer to the top of the tooth root). The periodontal pocket is a sure sign of periodontal disease.
Gingival sulcus is available for cleaning with standard toothbrushes and dental floss. On the other hand, gingival and periodontal pockets, due to their depth and inaccessibility, require professional cleaning by the dentist.
Treatment of periodontal disease
Therapy of periodontal disease can be conservative or surgical. The approach of treatment will depend on the degree of disease progression.
 Conservative treatment of periodontal disease involves removal of soft and firm deposits (dental plaque, calculus), conservative treatment of periodontal pockets (so-called curettage), but also training the patient about proper and regular oral hygiene maintenance and mandatory checkups. At the controls, the status of tooth-supporting apparatus (periodontium) is monitored and it is decided on further treatment on the basis of clinical examination and analysis of X-ray images.
Conservative treatment of periodontal disease involves removal of soft and firm deposits (dental plaque, calculus), conservative treatment of periodontal pockets (so-called curettage), but also training the patient about proper and regular oral hygiene maintenance and mandatory checkups. At the controls, the status of tooth-supporting apparatus (periodontium) is monitored and it is decided on further treatment on the basis of clinical examination and analysis of X-ray images.
In the surgical treatment of periodontitis, there are several different interventions, aimed at calming symptoms of periodontal disease and control of the further progression of the disease. The most common is the surgical treatment of periodontal pockets (so-called flap surgery) with the possible use of artificial bone substitutes, correction of soft tissue anomalies (gingivectomy, removal of blister and frenulum, free mucosal autograft, a connective tissue graft, treatment of recession with the use of Straumann Emdogain preparation).
It should be noted that without good cooperation with the patient, none of the mentioned therapeutic methods will have a full effect and can compromise the success of treatment. Daily and proper maintenance of oral hygiene (tooth brushing, use of dental floss, interdental brushes, antiseptic solutions, antiseptic agents) and regular controls (2 to 4 times a year) are necessary so we could together keep your teeth.

What happens to the gums in pregnancy?
The appearance of gingivitis (inflammation of gums) during pregnancy is not a rare occurrence. Redness, swelling and bleeding gum are the most common symptoms pregnant women notice. To this, primarily, comes due to a major change in the woman’s hormonal status, but also because of changes in everyday habits (more frequent meals, neglecting oral hygiene, irregular visits to the dentist). It should be emphasized that these changes are most often reversible (passing) character and can be controlled by regular maintenance of oral hygiene and more frequent visits to the dentist for control, removing soft and firm deposits, etc.
Can parodontopathy affect health at all?
Studies suggest a possible link between heart disease, lung diseases, diabetes, premature labor, reduced weight of the baby at birth and periodontal disease.
Is parodontopathy an infectious disease?
Periodontal disease is not a contagious disease in the true sense of the word. Although each of the additional factors for the occurrence of periodontal disease is individual and related to one person, there is still evidence that, through the saliva, the bacteria that cause this disease can be transferred from parents to children and among the couples.
